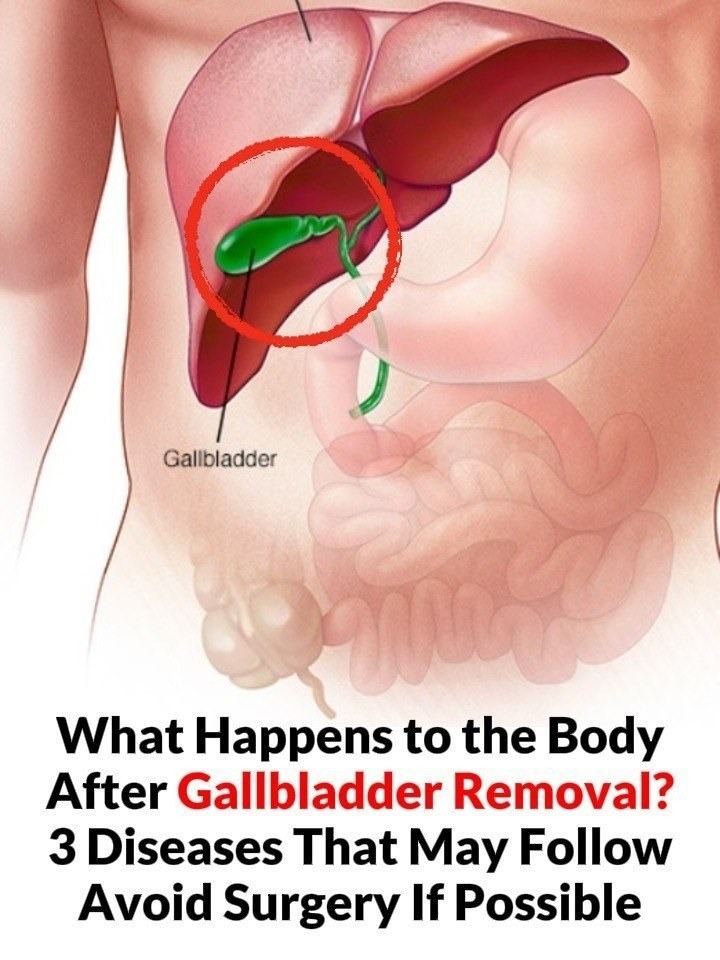
Gallbladder removal—called cholecystectomy—is one of the most commonly performed surgeries worldwide. It is usually done for gallstones, inflammation, or blocked bile flow.
What many people don’t realize is that the gallbladder is not essential for survival, but it does play a role in how smoothly your digestive system handles fats. When it’s removed, the body adapts—but that adaptation is not always perfect.
Below is a clear, detailed explanation of what actually changes in the body and the 3 main conditions that can sometimes follow surgery.
🧠 1. What the Gallbladder Normally Does
Your liver continuously produces bile. The gallbladder:
- Stores bile between meals
- Concentrates it (makes it stronger)
- Releases a “burst” of bile when you eat fatty food
👉 Think of it like a storage tank + controlled pump system
🩺 2. What Changes After Removal
After gallbladder removal:
- Bile has no storage space
- It flows directly from liver → intestine
- Release becomes continuous and low-pressure
This leads to three major physiological changes:
🔻 A. Less efficient fat digestion (at once)
You can still digest fats—but large fatty meals may overwhelm the system.
🔻 B. Constant bile exposure in intestines
Instead of timed release, bile trickles all day.
🔻 C. Gut adaptation over time
Most people adjust within weeks to months.
⚠️ 3. Conditions That May Follow Surgery
Not everyone gets these, but they are the most recognized post-surgery problems.
1. Postcholecystectomy Syndrome (PCS)
postcholecystectomy syndrome
This is an umbrella term, not one disease.
Symptoms may include:
- Upper abdominal pain
- Bloating and gas
- Nausea after eating
- Fat intolerance
- Heartburn-like discomfort
Why it happens:
- Remaining bile duct issues
- Sphincter of Oddi dysfunction (valve controlling bile flow)
- Acid reflux overlap
- Gut sensitivity after surgery
👉 Important: PCS affects a minority of patients, not most.
2. Bile Acid Diarrhea
bile acid diarrhea
This is one of the most common long-term changes.
What happens:
- Too much bile reaches the colon
- It irritates the bowel lining
- Water is pulled into the intestine → diarrhea
Symptoms:
- Loose stools (often after meals)
- Urgency to go to toilet
- Worsening after fatty foods
Key point:
This is often treatable with bile-binding medications or diet changes.
3. Small Intestinal Bacterial Overgrowth (SIBO)
small intestinal bacterial overgrowth
What happens:
After surgery, bile flow changes can slightly alter gut defenses.
Possible effects:
- Bloating and distension
- Excess gas
- Irregular bowel habits
- Food intolerance (especially carbs)
Important nuance:
SIBO is not caused only by gallbladder removal, but surgery can be one contributing factor in susceptible people.
4. Bile Reflux Gastritis
bile reflux gastritis
What happens:
Instead of staying in the intestine, bile sometimes flows backward into the stomach.
Symptoms:
- Burning upper abdominal pain
- Nausea (often worse on empty stomach)
- Bitter taste in mouth
- Chronic irritation of stomach lining
📊 4. So How Common Are These Problems?
Most studies show:
- 70–85% of people: no major long-term issues
- 10–20%: mild digestive symptoms that improve
- 5–10%: persistent or treatable complications
So complications exist—but they are not the norm.
🚫 5. “Avoid Surgery If Possible” — When This Is Misleading
It’s true in one sense:
- Surgery is not the first step for every gallstone case
- Mild or asymptomatic stones can sometimes be monitored
But it becomes dangerous advice when:
- Gallbladder is inflamed or infected
- Stones block bile ducts
- There is risk of pancreatitis
- Recurrent severe attacks occur
In these cases, delaying cholecystectomy can lead to serious complications.
🧾 6. The Real Bottom Line
- Your body can function without a gallbladder
- Digestion changes, especially fat handling
- A small group develops:
- Postcholecystectomy syndrome
- Bile acid diarrhea
- SIBO-related symptoms
- Bile reflux gastritis
- Most people adapt well over time
If you want, I can also explain:
- How to reduce side effects after surgery
- Which foods to avoid in the first 1–3 months
-
Or whether gallbladder surgery is usually avoidable in your specific situation (based on symptoms or reports)